The Polish Labour Code contains similar provisions.
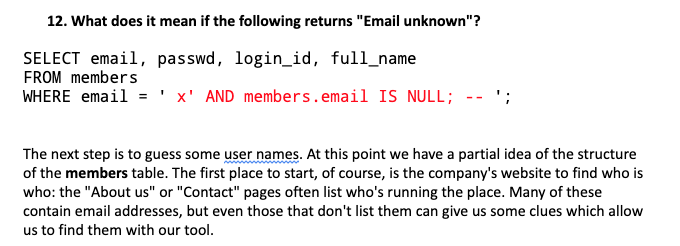
In the ED, we anticipate 100% of our patients will have a difficult airway. In a 2015 study, 93% of difficult airways were unanticipated. VL devices excelled especially in patients with known or predicted difficult airway. The downsides - most intubations were were performed by anesthesiologists in the OR, not the ED, and device use could not be blinded. They did not find harm associated with VL. In subgroup analysis, the Storz C-MAC reduced failed intubation more than other VL devices. There was heterogeneity among the RCTs, with 9 VL devices used. Odds of having no glottic view were reduced by 82% with VL (OR 0.18, 95%CI 0.13-0.27). Odds of an easy view of the glottic opening were 677% greater for VL over DL (OR 6.77, 95%CI 4.17-10.98). Authors said the NNT was 14 (not sure why the difference). For every 17 intubations, this means one less failed intubation. In the original study, the absolute risk of failed airway was 9.4% with DL, 3.5% with VL ARR = 0.094 - 0.035 = 0.059 1/ARR = NNT = 17. Use of VL vs DL reduced the number of failed intubations. This was a meta-analysis of 7044 patients in 64 RCTs, only 3 of which were based in the ED. Levitan says don’t choose VL or DL - use one that does both

Yet a Cochrane review in 2016 found VL had big advantages. The FELLOW, MACMAN, ED-based RCT, and dubious meta-analysis all found that VL did not improve first pass success over DL. For every 17 intubations using VL, one less patient will have a failed intubation. Video laryngoscopy (VL) gets the green light from Academic Emergency Medicine over direct laryngoscopy (DL) - clear benefit, no harm.